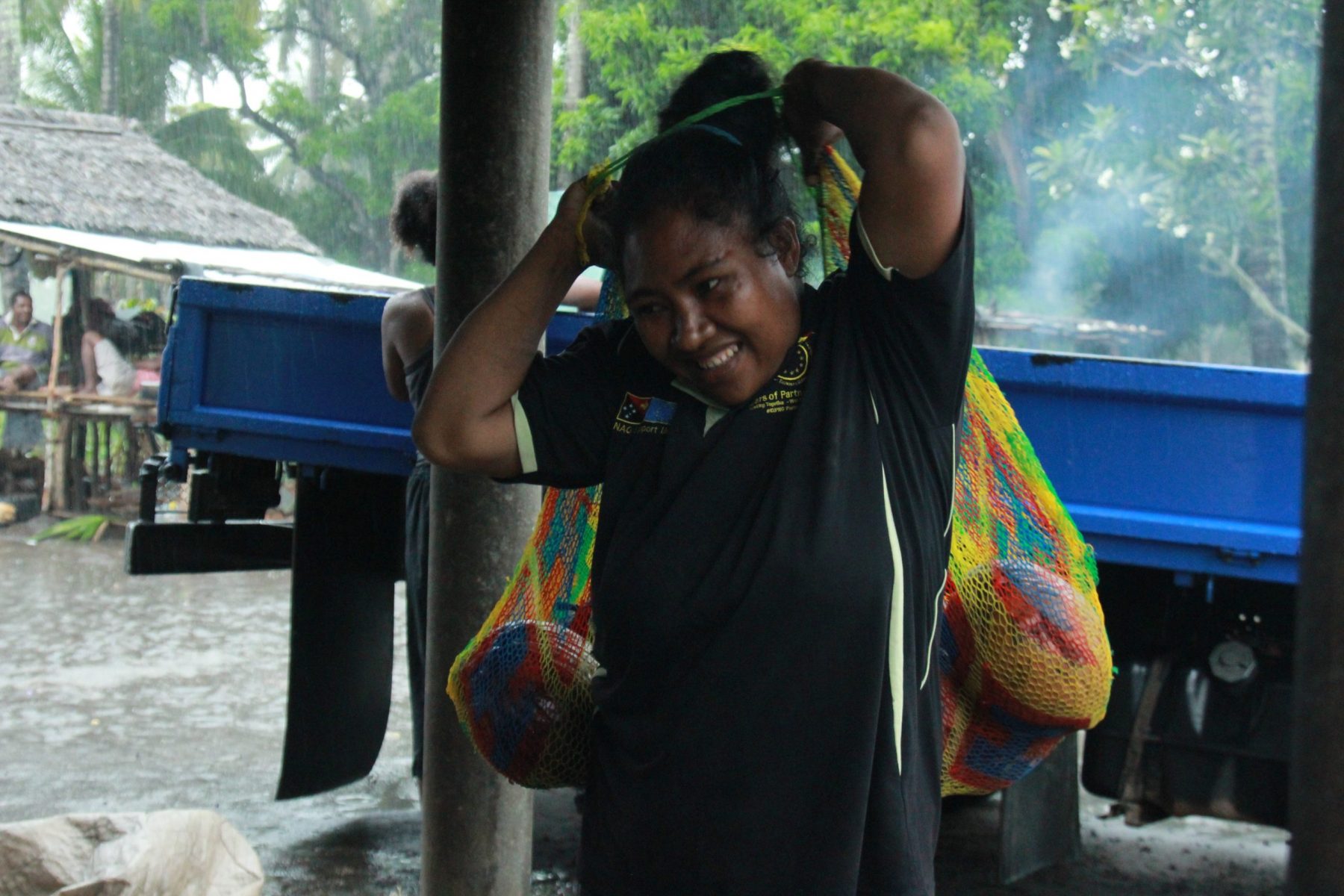A mother’s determination to save her children
Every other day Esther makes the same 8km walk to an under-resourced health centre with her two ill children. Her unrelenting determination reveals the lengths parents in Papua New Guinea must go to in search of basic, life-saving medical attention.
By Joe Flynn
A tropical downpour pounds Esther’s umbrella as she embarks upon the familiar walk to the health clinic 8km from her home in remote Central Province, Papua New Guinea.
In her arms she carries her one-year-old son Max, who has had a persistent cough for so long that Esther cannot remember when it first appeared. By her side is her 11-year-old daughter Ruth, who’s nursing a pair of swollen glands that will not go down.
It’s a long journey. It is one Esther has taken frequently since Max was born.
Searching for Answers
Like many mothers in Papua New Guinea, Esther knows the signs of tuberculosis. Papua New Guinea has one of the highest rates of tuberculosis in the world. In 2018, the country had more than 37,000 tuberculosis patients. Australia, a country with three times Papua New Guinea’s population, had just 1,700. Children in Papua New Guinea are particularly vulnerable.
Worldwide, one in 10 people with tuberculosis is a child. In Papua New Guinea, it is one in four.
These figures may not even paint the full picture. Many children with tuberculosis do not appear in the statistics because they are never diagnosed.

Life in remote Papua New Guinea
The health clinic that Esther goes to does not have the technology to diagnose tuberculosis. The closest place she can get her children diagnosed is Port Moresby, which is a three-hour drive away.
To get her children treated Esther has to pay to travel to Port Moresby and find a place for her family to stay there for up to a week.
This puts a huge burden on Esther’s family.
Despite these challenges, Esther estimates that she has made the trip to Port Moresby at least 10 times since Max was born. And she still does not have answers. She has vowed to continue making the journey until her children get better.
“It’s exhausting,” Esther said. “All I want is for my child to get better so I can get some rest.
“They’re my children. That’s why I keep going. I want them to be better. I feel like if I don’t get them to the hospital when they’re sick they might die.”

Unfortunately, many parents in Papua New Guinea have walked in Esther’s shoes.
Many people live long distances from their nearest functional health facilities, which are often struggling against the odds and unable to fulfil basic functions. Doctors are extremely scarce, particularly in rural areas, and the health workforce overall is only a fraction of the firepower required to maintain even basic programs.
In ChildFund’s experience working in Central Province, health clinics are often of such sub-standard quality that families can be forced to seek treatment in Port Moresby, if they are able to afford the costs of travelling. If not, which is most often the case, they remain undiagnosed, at risk of infecting other members of their community and potentially dying of a treatable disease.
“TB is quite difficult to diagnose in children unless someone is really skilled,” said Olive Oa, ChildFund Papua New Guinea’s Health Programs Manager. “It cannot be diagnosed by a community health worker. Children can really suffer before they are diagnosed; they will gradually lose weight, they won’t be able to play with their friends, they won’t be able to eat properly.”
When the disease is not treated many children die. “Children, their immune system is not usually as strong as adults so it will usually make them weaker and they will get sicker and if you don’t find treatment quickly they may get sick and they may die – but it will take time,” Olive said.
“If you don’t find treatment quickly they may get sick and they may die.”
Olive, who saw firsthand the damage of an undiagnosed case of tuberculosis when her son lost half his body weight while battling with the disease as a teenager, is committed to ending tuberculosis in Papua New Guinea.
She oversees ChildFund’s health programs, which work in partnership with healthcare workers, children and their families in remote villages in Papua New Guinea to help children like Max and Ruth.

Help end infectious diseases like TB in PNG
“They’re my children. That’s why I keep going. I want them to be better.” – Esther, mother of Max and Ruth
These programs help children in remote communities get diagnosed and treated for tuberculosis, which is saving lives.
Early this year, Olive saw Esther and her children outside their local clinic. Ruth’s swollen glands stood out immediately. Then she noticed Max’s cough. Olive asked Esther if anyone else in the house had been coughing. Esther told her that her father had been coughing a lot.
None of them have been diagnosed with tuberculosis. Esther took Max to get tested in Port Moresby, but she got scared when she learnt the doctor wanted to stick a tube down her son’s throat.
After being reassured by Olive, Esther vowed to take Max back to Port Moresby and let them take a sample of his sputum so he could be tested for tuberculosis. Ruth was also tested in Port Moresby but the results did not show signs of tuberculosis. Olive knows the disease is hard to diagnose. Her son was not diagnosed for six months despite seeing several doctors. Esther said she would also get Ruth tested again.
Until the children can get diagnosed and treated for their illnesses, they are extremely vulnerable. Olive is worried about how the family will fare.
“Max keeps having recurrent chest infections,” Olive told us. “He looks like he is wasting a bit and is continuously coughing. Ruth has very enlarged lymph nodes and neither of them are the normal weight for their age.”
“I think (Esther) probably feels how I felt when my son was getting sick; you know I would just go up and down, you would just want everything to be good for your children, the child to be better so you feel good and not stressed. You come home and the child is sick. I think she’s quite stressed.”